Lung Cancer Awareness Month
Story by Cheri Woodsmall
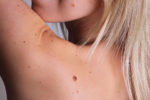
When Julia started feeling worn down and tired after working in her garden for a couple of hours, she knew that there was something amiss. She was an athletic 52-year-old that took pride in her health and made a conscious effort to eat well, avoid smoking, and only drink alcohol on special occasions. It was when she began coughing up a bit of blood that prompted her to schedule a visit to her primary care doctor. That visit changed her life. Two days later, she received the news that she had Stage-4 Lung Cancer.
SYMPTOMS
Most lung cancers do not cause any symptoms until they have spread, but some people with early lung cancer do have symptoms. If you go to your doctor when you first notice symptoms, your cancer might be diagnosed at an earlier stage, when treatment is more likely to be effective.
Most of these symptoms are more likely to be caused by something other than lung cancer. Still, if you have any of these problems, it’s important to see your doctor right away so the cause can be found and treated, if needed.
The most common symptoms of lung cancer are:
- A cough that does not go away or gets worse
- Coughing up blood or rust-colored sputum (spit or phlegm)
- Chest pain that is often worse with deep breathing or coughing
- Hoarseness
- Loss of appetite
- Unexplained weight loss
- Shortness of breath
- Feeling tired or weak
- Infections such as bronchitis and pneumonia that don’t go away or keep coming back
- New onset of wheezing
If lung cancer spreads to other parts of the body, it may cause:
- Bone pain (like pain in the back or hips)
- Nervous system changes (such as headache, weakness or numbness of an arm or leg, dizziness, balance problems, or seizures), from cancer spread to the brain
- Yellowing of the skin and eyes (jaundice), from cancer spread to the liver
- Swelling of lymph nodes (collection of immune system cells) such as those in the neck or above the collarbone
WHAT CAUSES LUNG CANCER?
We don’t know what causes each case of lung cancer. But we do know many of the risk factors for these cancers and how some of them cause cells to become cancer.
SMOKING
Smoking tobacco is by far the leading cause of lung cancer. About 80% of lung cancer deaths are caused by smoking, and many others are caused by exposure to second-hand smoke.
Smoking is clearly the strongest risk factor for lung cancer, but it often interacts with other factors. People who smoke and are exposed to other known risk factors such as radon and asbestos are at an even higher risk. Not everyone who smokes gets lung cancer, so other factors like genetics probably play a role as well.
Not all people who get lung cancer smoke. Many people with lung cancer formerly smoked, but many others never smoked at all. And it is rare for someone who has never smoked to be diagnosed
with small cell lung cancer (SCLC), but it can happen.
WAIT, JULIA DIDN’T SMOKE
Lung cancer in people who don’t smoke can be caused by exposure to radon, secondhand smoke, air pollution, or other factors. Workplace exposures to asbestos, diesel exhaust or certain other chemicals can also cause lung cancers in some people who don’t smoke.
A small portion of lung cancers develops in people with no known risk factors for the disease. Some of these might just be random events that don’t have an outside cause, but others might be due to factors that we don’t yet know about.
Lung cancers in people who don’t smoke are often different from those that occur in people who do. They tend to develop in younger people and often have certain gene changes that are different from those in tumors found in people who smoke. In some cases, these gene changes can be used to guide treatment.
DIAGNOSIS
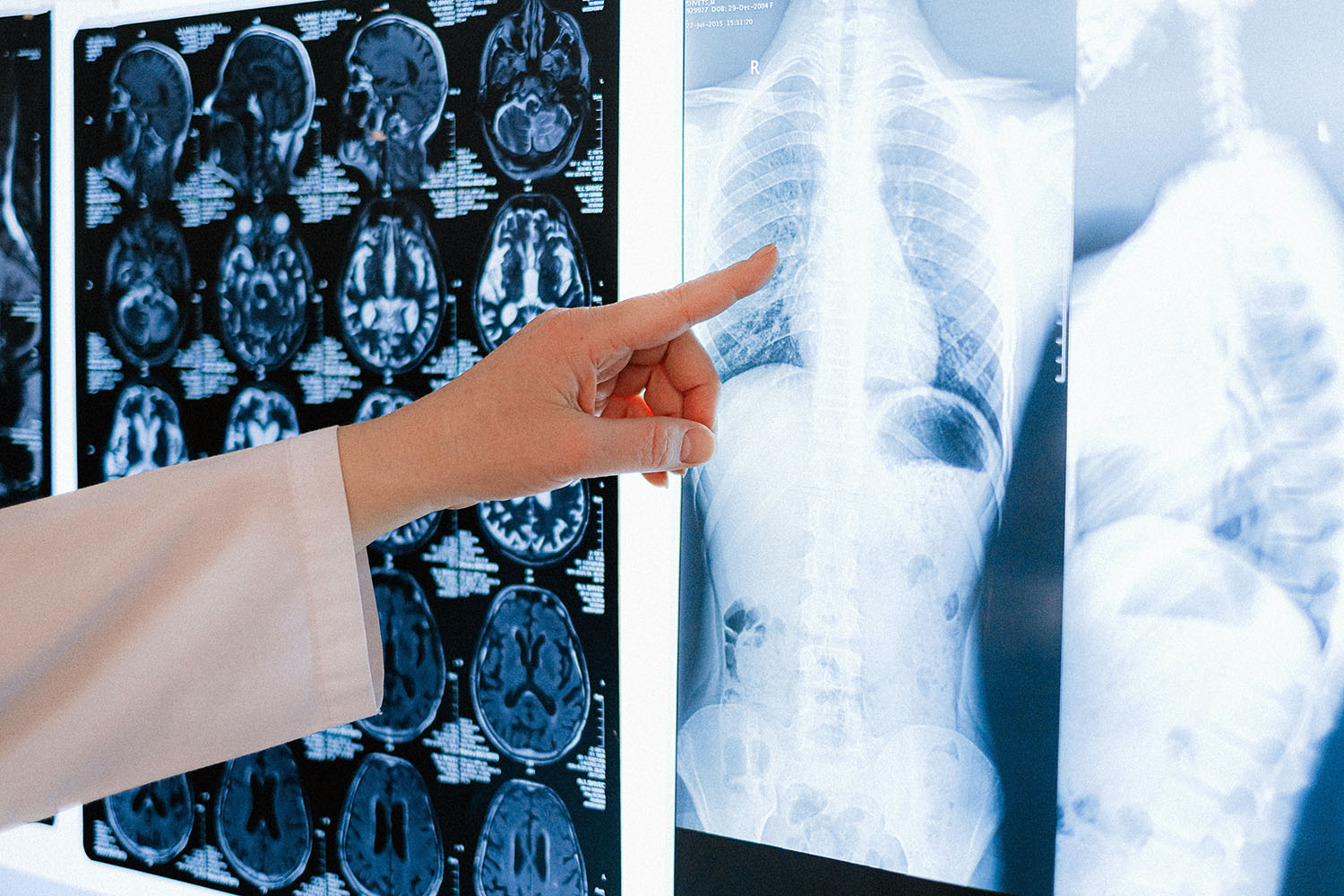
If there’s reason to think that you may have lung cancer, your doctor can order several tests to look for cancerous cells and to rule out other conditions.
Tests may include:
- Imaging tests. An X-ray image of your lungs may reveal an abnormal mass or nodule. A CT scan can reveal small lesions in your lungs that might not be detected on an X-ray.
- Sputum cytology. If you have a cough and are producing sputum, looking at the sputum under the microscope can sometimes reveal the presence of lung cancer cells.
- Tissue sample (biopsy). A sample of abnormal cells may be removed in a procedure called a biopsy.
Careful analysis of your cancer cells in a lab will reveal what type of lung cancer you have. Results of testing can tell your doctor the specific characteristics of your cells that can help determine your prognosis and guide your treatment.
Tests to determine the extent of the cancer:
Once your lung cancer has been diagnosed, your doctor will work to determine the extent (stage) of your cancer. Your cancer’s stage helps you and your doctor decide what treatment is most appropriate.
Staging tests may include imaging procedures that allow your doctor to look for evidence that cancer has spread beyond your lungs. These tests include CT, MRI, positron emission tomography (PET) and bone scans. Not every test is appropriate for every person, so talk with your doctor about which procedures are right for you.
The stages of lung cancer are indicated by Roman numerals that range from 0 to IV, with the lowest stages indicating cancer that is limited to the lung. By stage IV, the cancer is considered advanced and has spread to other areas of the body.

TREATMENT OPTIONS
Depending on its type and stage, lung cancer may be treated with surgery, chemotherapy or other medications, radiation therapy, local treatments such as laser therapy, or a combination of treatments. Combination treatment or multimodality treatment refers to having more than one type of treatment.
Treatment for lung cancer includes one or more of the following approaches.
SURGERY
Surgery is part of the treatment for early-stage lung cancers. The type of surgery depends on the size and location of the tumor in the lung, the extent of the cancer, the general health of the patient and other factors. Many surgeries are done with a long incision in the side of the chest, known as a thoracotomy. Some early-stage tumors may be treated with video-assisted thoracic surgery (VATS), which uses several small incisions (instead of one large one) and special long surgical tools.
RADIATION THERAPY
Radiation therapy is the use of high-energy radiation to kill cancer cells and shrink tumors. Radiation may also be used with chemotherapy to treat lung cancer.
CHEMOTHERAPY
Whereas surgery and radiation treatment are focused on only one area of the body, chemotherapy goes throughout the body to search for tumor cells. Chemotherapy is given through an IV infusion, in most cases, chemotherapy works by interfering with the cancer cells’ ability to grow or reproduce. Different groups of drugs work in different ways to fight cancer cells. The oncologist will recommend a treatment plan for each individual. Chemotherapy may be given before other treatments, after other treatments, or alone for lung cancer.
IMMUNOTHERAPY
Immunotherapy is a new cancer treatment approach that uses drugs, vaccines, and other therapies to activate the immune system’s natural defenses so it can fight cancer. One type of immunotherapy drug, called “anti-PD-1” has been shown to cause significant tumor regression in a quarter of patients who receive it after a round of chemotherapy. Three immunotherapy drugs —pembrolizumab, atezolizumab, and nivolumab — have been approved to treat certain non-small cell lung cancers.
LOCAL SUPPORT
Gilda’s Club Kansas City 816.531.5444 | gildasclubkc.org
University of Kansas – Go2 Foundation for Lung Cancer | 913-574-2712
American Lung Association in Kansas 913-353-9165 | lung.org
Sources: cancer.org, WebMD, John’s Hopkins Medicine, MayoClinic, KU Med