Healing, Comfort and Hope Meet Modern Technologies

As an interventional physiatrist, C. Lan Fotopoulos, M.D. specializes in minimally-invasive and interventional procedures for back, neck, hip, shoulder and knee pain.
Story by Ann Butenas | Sponsored Content

If hip, neck, back, shoulder or knee pain are chronically weighing you down, then you should strongly consider the medical services of Dr. C. Lan Fotopoulos with Dickson-Diveley Orthopaedics, which has locations at the Kansas City Orthopaedic Institute in Leawood and on the Saint Luke’s Hospital campus in Kansas City, Missouri. A skilled, respected, experienced and in-demand interventional physiatrist, Dr. Fotopoulos stands among an elite group of orthopedic physicians whose contribution to the field of orthopedic medicine involves personalized care across all subspecialties in orthopedic medicine using state-of-the-art technologies coupled with the best in patient care.
Dr. Fotopoulos fully understands how pain affects people, and his primary goal is to alleviate such pain to the degree that he can with whatever methods are deemed appropriate for the patient and the situation. He entered into orthopedics primarily because he wanted to help people live better and lead more productive lifestyles. As an interventional physiatrist, he knows what to do to help people return to their lives, their livelihoods and their loved ones. But it is the patient testimonials that really get to the heart of who Dr. Fotopoulos is…
“Dr. Fotopoulos is extremely attentive and always makes me feel important. He listens and I know he cares.” ~ Kara W.
Dr. Fotopoulos was excellent in his thorough exam and communication of my problem and the next steps we should take to resolve my neck injury.” ~ David N.
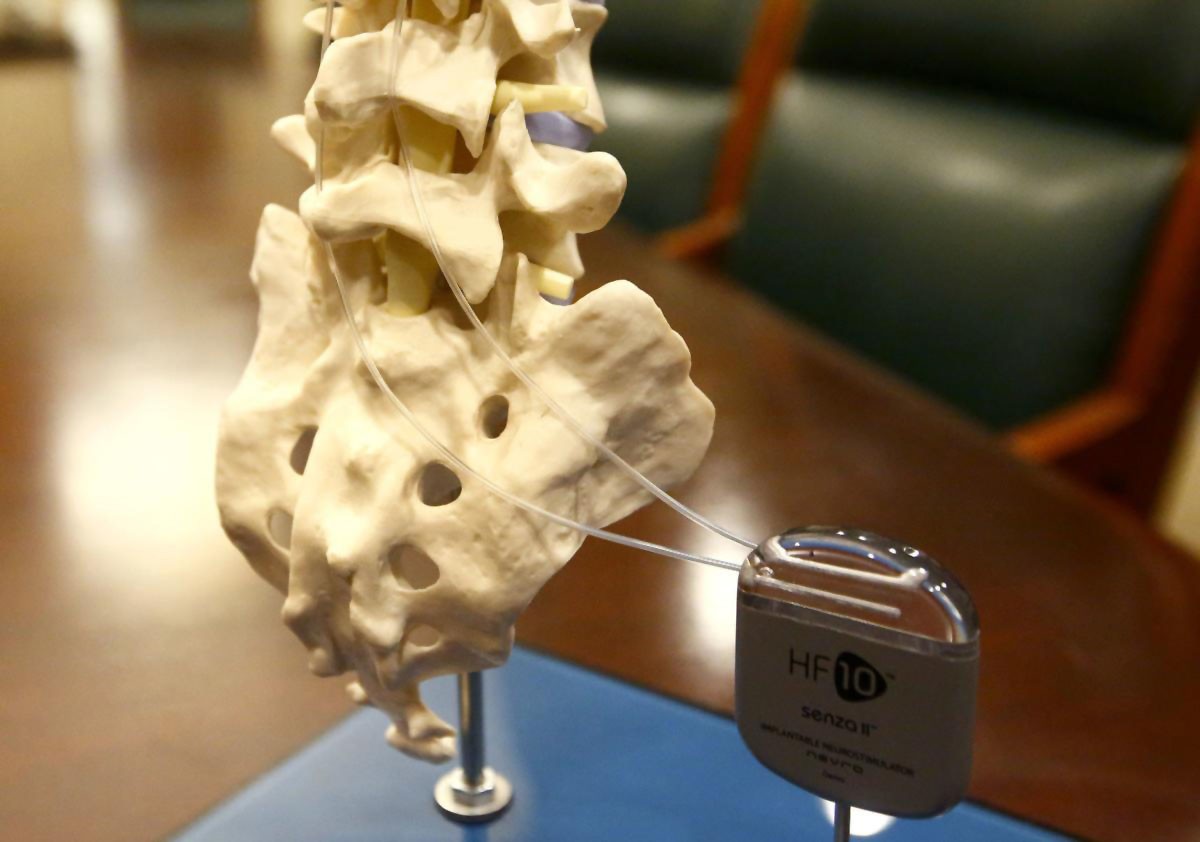
Relief from Painful Diabetic Neuropathy: A New Direction for Spinal Cord Stimulation
Spinal cord stimulation involves an implanted device that transmits mild electrical impulses to the spinal cord. As a result, the feelings of pain are interrupted, giving the patient the opportunity to enjoy pain relief in such a way that it does not interfere with activities of daily living. Spinal cord stimulation has been used for decades as a way to greatly reduce or perhaps even eradicate the use of pain medication. This is great news for individuals who do not want to rely on pain killers or who fear the potential unwanted dependence on them.
Dr. Fotopoulos can also perform procedures after other surgeries have already been done or perhaps were ineffective, such as those related to chronic neck pain or low back pain with radiating pain down the leg which has not been cured with surgery. He often implements spinal cord stimulation, which stimulates the spinal cord with a small pulse that can relieve most, if not all pain, without surgery.
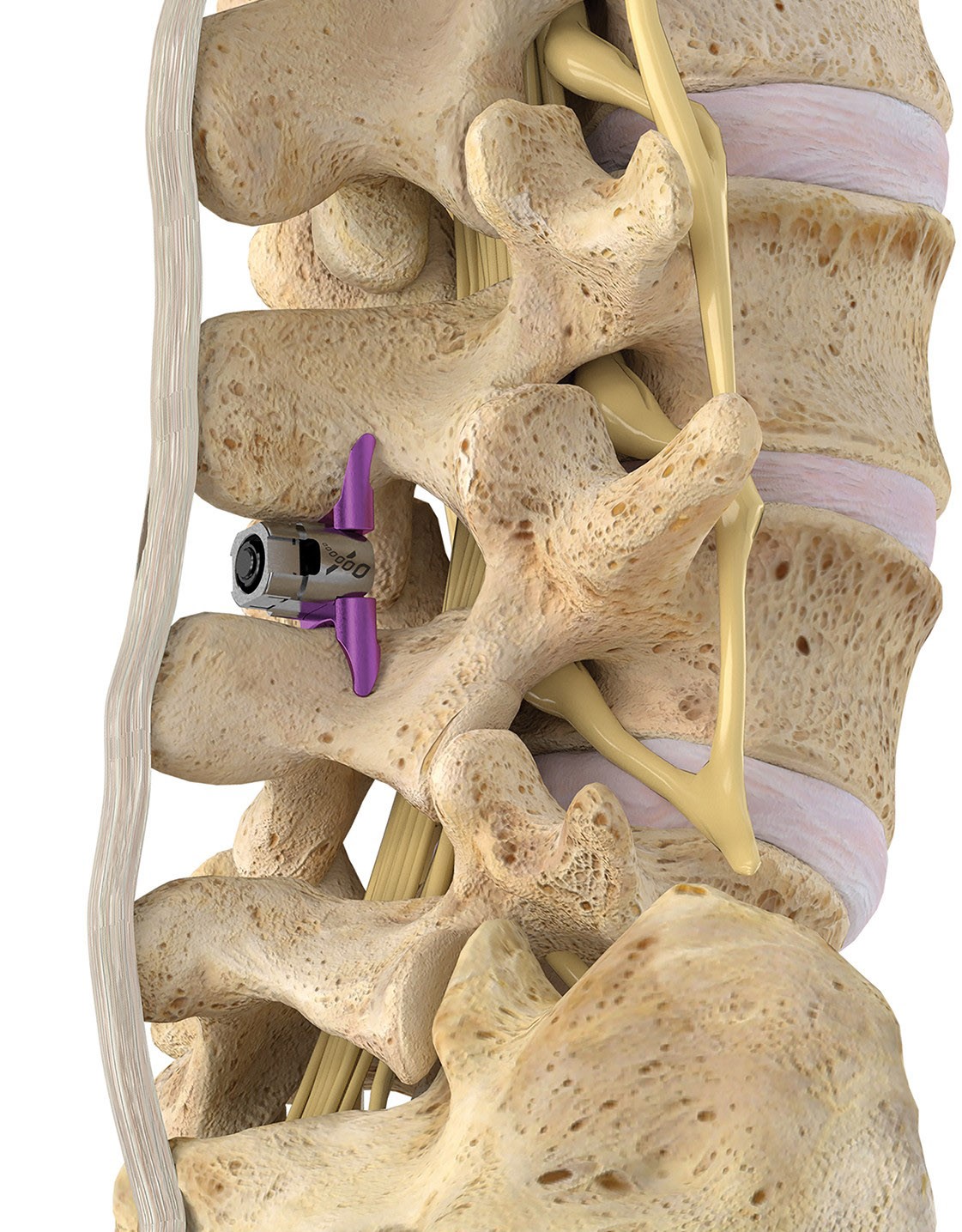
The Vertiflex® Procedure: “Revolutionizing the Treatment of Spinal Stenosis”
If you or someone you know suffers from lumbar spinal stenosis, you know how debilitating it can be. You may not be able to pursue the once-active lifestyle you enjoyed due to chronic pain, cramping, weakness and/or numbness, and as a result, comfort and mobility can be adversely affected. While medication, physical therapy and surgery are all potentially viable methods of treatment, sometimes these do not provide the necessary relief patients need.
While there are several treatment options available for lumbar spinal stenosis, including over-the-counter non-steroidal anti-inflammatory drugs, heat, massage therapy, spinal injections and physical therapy, spine surgery may be considered if those non-operative therapies are ineffective or if a patient’s symptoms continue to progress. Many patients, however, cannot tolerate the more invasive approaches or simply are not good candidates for such therapies. Thanks to a new treatment option known as the Vertiflex Procedure, many patients are discovering the joy that comes with getting back to doing the things they love to do most with the least amount of disruption to their lives as possible.
The Vertiflex® device is placed between the posterior aspects (back part) of the spine, preventing the extension of the spine while still providing room for flexion. This opens up the space and allows for the pain to be resolved.
Dorsal Root Ganglion Stimulation: Exciting New Treatment for Individuals Suffering from Chronic Pain
Dr. Fotopoulos has been specifically appointed by St. Jude Medical, Inc., a global medical device company and international leader in the development of therapies for the treatment of chronic pain, to be trained with the use of the St. Jude Medical Axium Neurostimulator System. Clinically described, this system “targets the dorsal root ganglion (DRG), a spinal structure densely populated with sensory nerves that transmit information to the brain via the spinal cord.” This device allows for spinal stimulation that can target specific areas of the body where pain occurs. Using this device, patients can receive effective pain relief for certain neuropathic conditions that otherwise might not be achieved by traditional spinal cord stimulations.
“The perfect candidate for this procedure is someone who is experiencing unrelieved pain from such conditions as previous knee surgery; pain after knee replacement surgery; unresolved pain issues from foot and ankle surgeries; post-hernia pain or hip replacement surgery,” noted Dr. Fotopoulos. “This procedure allows localized stimulation, treating complex regional pain syndrome, also known as sympathetic dystrophy.”
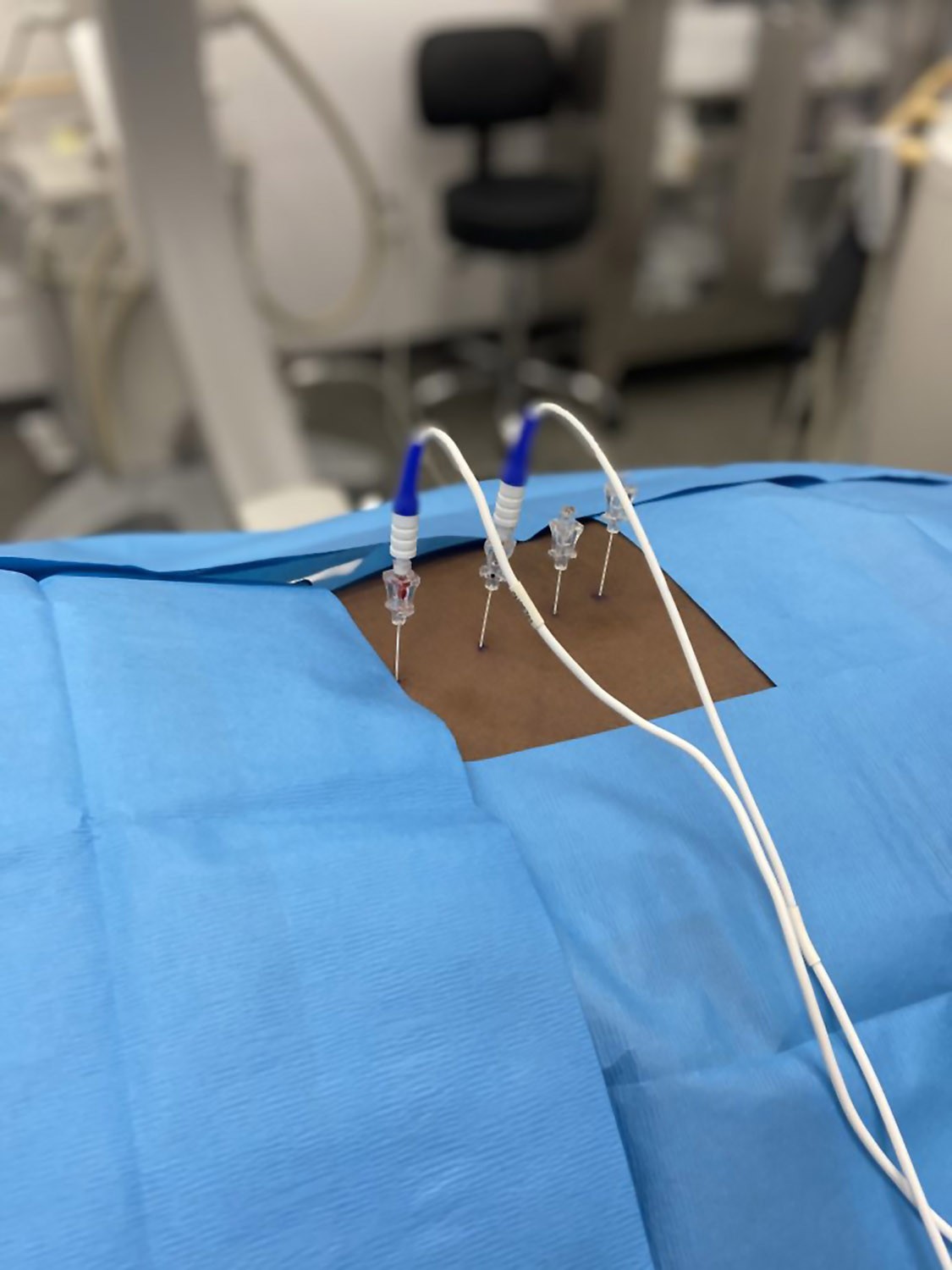
Radiofrequency Ablation: A Potential Answer for Chronic Low Back Pain, Knee Pain and Even Certain Types of Headaches
Radiofrequency ablation is a minimally invasive procedure used to destroy the nerve fibers that carry pain signals to the brain. Dr. Fotopoulos emphasized not everyone with back pain or neck pain needs a steroid. He noted there’s a very large number of patients for which other treatments are beneficial, such as radio frequency ablation, which helps with whiplash, headaches and even knee pain.
“Through the use of radiofrequency ablation, we use heat produced by radio waves to cauterize sensory nerves in the body,” explained Dr. Fotopoulos. “In addition to treating low back pain, neck pain and headaches, this type of procedure has also been used for tumors as well as for certain cardiac issues. It can provide relief for patients struggling with chronic pain, especially in the neck and lower back.”
In the pain world, when discussing chronic back and neck pain, physicians refer to the facet joints, which are located in the back of the spine. These are the joints that make your back flexible and allow you to bend and twist. The nerves exit your spinal cord via these joints on their way to other parts of the body. Just like other joints, they have a capsule around them, cartilage, and fluid. They are also susceptible to arthritis. A healthy facet joint enables the vertebrae to move smoothly against each other without grinding. Facet joint syndrome results when there is pain at the joint between two vertebrae in the spine. This is also known as osteoarthritis. When these joints become swollen and painful, it is called facet joint syndrome.
The diagnosis of facet joint syndrome is a history-based exam. Simultaneous to ruling out fractures and herniated discs, a physical examination and complete patient history is taken. Prior to the actual procedure of radiofrequency ablation, the patient will undergo a medical branch block under local anesthesia on the medial branch nerve to determine how he or she will respond. If the pain gets better, then sometimes a second block is done. If the patient responds favorably at that point, then typically a follow-up visit for the radiofrequency ablation is scheduled.
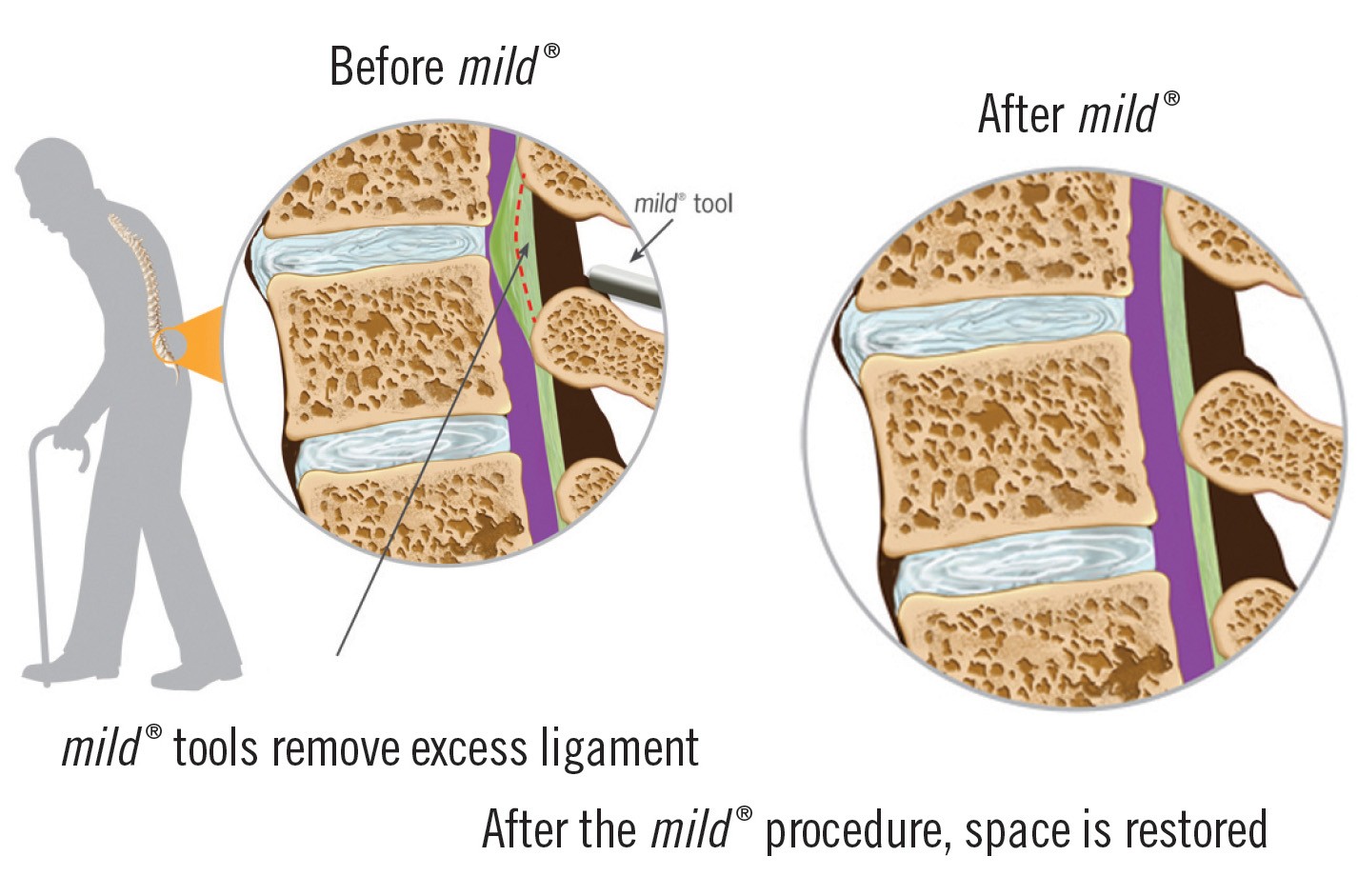
Now Available to Medicare Patients Nationwide, a procedure called mild® is Helping Lumbar Spinal Stenosis Patients Embrace Life Again.
As we age, our body goes through the natural wear and tear of life, and as a result, the spinal canal can become constricted due to increased ligament tissue, overgrown bone or bulging discs which create pressure on the spinal cord. When the spinal canal is narrowed in the lower part of the spine, this is referred to as lumbar spinal stenosis (LSS). This condition affects more than 1.2 million patients in the country. Patients may experience pain, numbness or tingling in the lower back, legs or buttocks. This can limit the individual’s ability to walk or stand for any appreciable length of time. LSS usually targets people over 50 years of age and the likelihood of developing it does increase with age. It is estimated that roughly 10% of Americans have lumbar spinal stenosis, and that by this year some 2.4 million will be experiencing considerable pain as a result of the condition.
Fortunately, there is a procedure called mild® (minimally invasive lumbar decompression), an FDA-approved and clinically proven outpatient procedure that can help patients diagnosed with LSS. Performed through a small incision about the size of a baby aspirin, mild® requires no stiches, is done under conscious twilight sedation as opposed to general anesthesia, involves no implants and requires no overnight hospital stay.
Essentially, mild® is designed to remove excess ligament tissue that is causing the narrowing of the spinal canal. Since it does not change the structural stability of the spine, open surgery can be performed on the patient later if necessary. As a result of mild®, patients are getting back to their lives again, as mobility has been restored, pain has been reduced, and the compression of nerves has been alleviated.
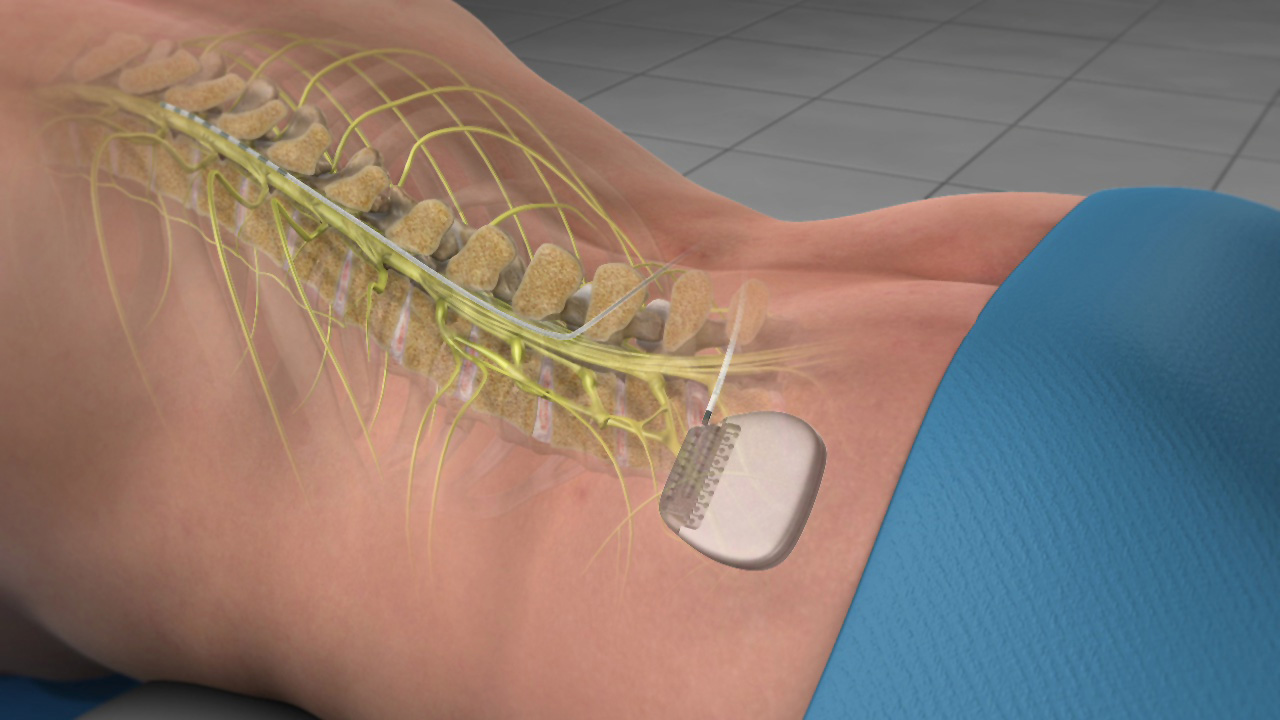
Spinal cord stimulation has historically been used for chronic pain of the trunk and limbs but a new ultra-high frequency platform is showing promise for relief from the pain of diabetic neuropathy.
When you think of nerve pain in your feet, your thoughts most likely don’t turn to treatment indications for your back. However, if you suffer from diabetic peripheral neuropathy, which can include sensations such as prickling, tingling, sharp pain, cramping, and/or deep stabbing pain in your feet typically associated with chronic high blood sugar, you could be a candidate for spinal cord stimulation as an alternative treatment protocol.
Spinal cord stimulation involves an implanted device that transmits mild electrical impulses to the spinal cord. As a result, the feelings of pain are interrupted, giving the patient the opportunity to enjoy pain relief in such a way that it does not interfere with activities of daily living. Spinal cord stimulation has been used for decades as a way to greatly reduce or perhaps even eradicate the use of pain medication. This is great news for individuals who do not want to rely on pain killers or who fear the potential unwanted dependence on them. This procedure does not mask or trick the brain in any way; it simply changes the character of the feelings of pain and discomfort patients may experience in their feet.
Vertebroplasty for vertebral compression fractures
Invented more than three decades ago, vertebroplasty is a procedure to treat back pain as a result of compression fractures using a large needle called a trocar which is placed through the bone into the fractured one. With vertebral augmentation, cement is inserted through the needle, essentially gluing together the fractured pieces. As a result, the fractures are immobile, providing the back pain relief to the patient.
Bottom line…
These represent just a few examples of the pain relief measures Dr. Fotopoulos can offer his patients. Knowing his patients are returning to their lives, getting healthy and leaving pain in the rearview mirror is what motivates Dr. Fotopoulos to continue to deliver the best in patient care.
“When I get a call that someone is not coming in (to the office) today because they feel great, I love that,” he smiled. “And when I have an 80-year-old patient who tells me he feels like he is 60 again, that is very heart-warming to hear.”

Saint Luke’s Hospital Campus Medical Plaza Building 1, Ste 610, 4321 Washington St., KCMO and at 3651 College Blvd, Leawood, KS 66211






