Relief from Painful Diabetic Neuropathy
A New Direction for Spinal Cord Stimulation While Working Under Stricter Guidelines During the COVID-19 Global Pandemic with Dr. Constantine Fotopoulos Dickson-Diveley Orthopaedics
Spinal cord stimulation has historically been used for chronic pain of the trunk and limbs but a new ultra-high frequency platform is showing promise for relief from the pain of diabetic neuropathy.
When you think of nerve pain in your feet, your thoughts most likely don’t turn to treatment indications for your back. However, if you suffer from diabetic peripheral neuropathy, which can include sensations such as prickling, tingling, sharp pain, cramping, and/or deep stabbing pain in your feet typically associated with chronic high blood sugar, you could be a candidate for spinal cord stimulation as an alternative treatment protocol. However, while living in the midst of a global pandemic, is access to such care even available at this time? Fortunately, there is a local medical expert who can provide the treatment and attention you need and who will judiciously employ every effort to ensure such treatment is delivered in accordance with global governance, requisite health and safety standards, and within a priority setting while keeping the best interests of the public health at top of mind.
A trusted local expert providing highly-personalized care in orthopedic medicine
A graduate of the University of Missouri- Kansas City School of Medicine, Dr. Constantine Fotopoulos is board-certified in physical medicine and rehabilitation, pain medicine, sports medicine and undersea hyperbaric medicine. Additionally, he has worked as an emergency room physician and also served as a lieutenant commander and diving and undersea medical officer in the United States Navy. He is currently a physician at Dickson-Diveley Orthopaedics, with locations in Leawood and in Kansas City at Saint Luke’s Hospital Campus Medical Plaza, where he specializes in spine and sports medicine. A skilled, respected, experienced and in-demand interventional physiatrist, Dr. Fotopoulos stands among an elite group of orthopedic physicians whose contribution to the field of orthopedic medicine involves personalized care across all subspecialties in orthopedic medicine using state-of-the-art technologies coupled with the best in patient care.

But how do you manage a chroniccondition while simultaneously dealing with the effects of a worldwide pandemic?
When the coronavirus, a/k/a COVID-19, began to gain ground and expand its coverage across the globe, it raised concerns for everyone, especially those who are older and/or who have pre-existing medical conditions. Caregivers, families and patients with neuropathy symptoms should practice diligence and adopt the precautionary measures such as self-quarantining and social distancing. These actions are vitally important to prevent the spread of the virus, not only to the patient, but also to those who care for the patient and for others with whom the patient may come in contact. The coronavirus brings with it new information almost on a daily basis, adding to its mysterious nature. Some commonly-now high-risk factors include heart disease, lung disease and diabetes. Neuropathy symptoms can be caused by diabetes. Therefore, it is important to not take any chances with potentially establishing contact with the virus.
How to take care of yourself and your disease during the coronavirus scare
First and foremost, wash your hands! Do this frequently. Avoid close contact with others to minimize the potential transfer of the virus. If you are a patient struggling with neuropathy, enlist a family member or caregiver to tend to all of your food shopping and other essential errands. Alternatively, consider having food and other grocery items delivered directly to your home. Essential items to have on hand as a patient and a caregiver includes masks, soap, hand sanitizer and disinfectant wipes.
Additionally, take care of yourself by maintaining a healthy diet and taking care of your mental health. While getting together with friends and extended family may not be an option, you can connect by phone, Skype or other software applications.
By exercising the aforementioned precautions, you may better position yourself to undergo treatment options for painful diabetic neuropathy while simultaneously taking positive actions to avoid contracting coronavirus.
Spinal cord stimulation explained
In a nutshell, spinal cord stimulation involves an implanted device that transmits mild electrical impulses to the spinal cord. As a result, the feelings of pain are interrupted, giving the patient the opportunity to enjoy pain relief in such a way that it does not interfere with activities of daily living. Spinal cord stimulation has been used for decades as a way to greatly reduce or perhaps even eradicate the use of pain medication. This is great news for individuals who do not want to rely on pain killers or who fear the potential unwanted dependence on them. Fortunately, there are trusted medical experts in the metro area who can consult with patients about this newly-directed procedure that does not mask or trick the brain in any way; it simply changes the character of the feelings of pain and discomfort patients may experience in their feet.
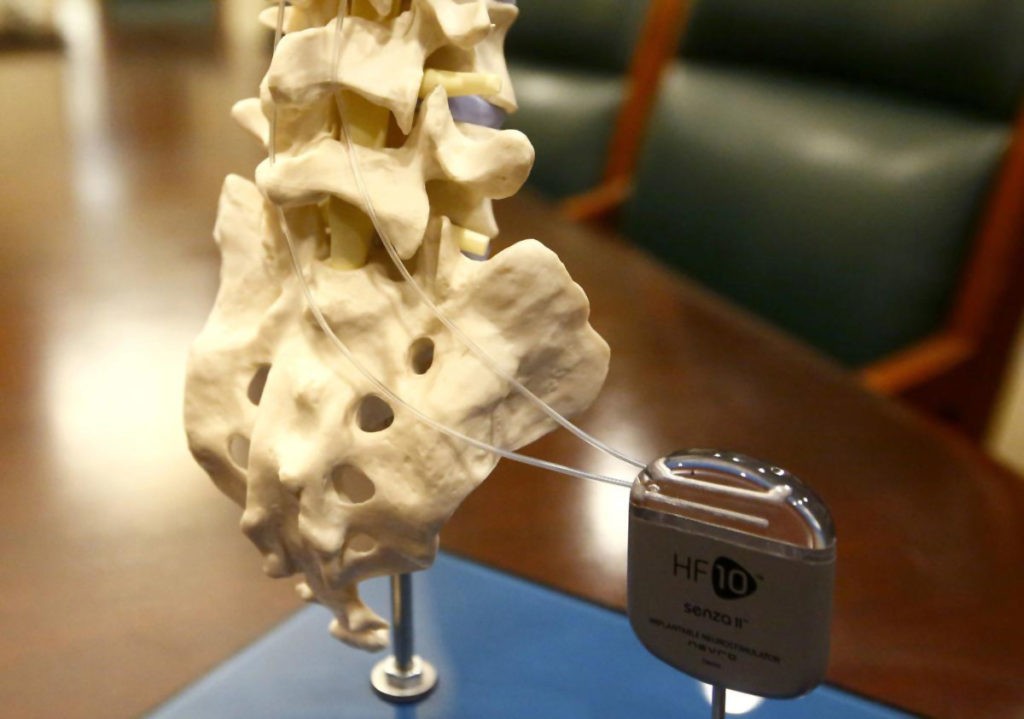
Taking Spinal Cord Stimulation in a New and Promising Direction
Spinal cord stimulation, which has been indicated for axial and limb pain and previously used for back surgery, back pain, non-operative back pain and sciatic pain, is currently in the process of securing approval for peripheral neuropathy. This new therapy, HF10, utilizes ultra-high frequency without the use of traditional paresthesia-based spinal cord stimulation systems.
“Peripheral neuropathy is nerve pain previously caused by scarring around nerves after surgery, from RSK, or nerve injury,” stated Dr. Fotopoulos. “This approach to using spinal cord stimulation is to treat nerve based pain in extremities of a different diagnosis. In the past, it was used to treat spine-related pain. Diabetic neuropathy is very common in those with Type 1 diabetes, especially end stage, and this offers a potentially successful treatment for patients for whom oral medications have proven ineffective.”
Done on an out-patient basis, this procedure does adhere to strict pre-operative standards. First, a consultation is done to determine if it is right for the patient. From that point, the patient is required to consult one time with a psychologist for an evaluation, as per insurance requirements. Upon successfully meeting those two requirements, the patient then undergoes a trial procedure.
“We percutaneously thread two wires up the epidural space into a certain area around the spine where the patient needs them and where we know it affects different pain centers,” stated Dr. Fotopoulos. “We leave it attached for seven to ten days as the patient goes about his or her daily routine. The purpose of this is to determine if it positively affects one’s daily life and restores more quality to that end. If it is successful and it works, then he or she is a candidate for a permanent system. However, we have them wait for two weeks to rule out any evidence of infection and will then surgically implant the device in a follow-up procedure. Through a remote control device, the patient can control and relieve pain so it does not interfere with his or her daily life.”
Dr. Fotopoulos prefers to see at least a 70%-80% reduction in symptoms before moving forward with the insertion of the permanent device, and depending on the clinic at which the patient undergoes this procedure, all of this can be potentially accomplished in a month’s time. Even though this device is considered permanent, it is a reversable treatment therapy and can be easily removed at any time.
Footnote
“This type of work is very rewarding when dealing with the chronic pain population,” expressed Dr. Fotopoulos. “When patients come to me who have tried other modalities and multi-faceted treatments with little to no improvement, this is where we can help.”
Most of the surgeries are performed at the Kansas City Orthopedic Institute, which is partially physician-owned. As a leading expert in this course of treatment, Dr. Fotopoulos knows which patients will do well with this system based on medical history and related complaints.
“We have a staff of experts in orthopedic care, from the front desk to the anesthesiologists,” said Dr. Fotopoulos. “As a result, we realize low infection rates and high patient satisfaction rates.”

Saint Luke’s Hospital Campus Medical Plaza Building 1, Ste 610, 4321 Washington St., KCMO and at 3651 College Blvd, Leawood, KS 66211
913.319.7678 ext 3109 | DD-Clinic.com