Hospice Houses Lead the Way in a Heart-Breaking Time of Pandemic

Story by Wanda Kelsey-Mendez
In March 2020, the first COVID nursing home death occurred in the Kansas City area and as a result, hospitals began limiting visitors and most skilled nursing facilities went on lockdown. The COVID Task Force at Kansas City Hospice & Palliative Care had already begun to write protocols and search for PPE. Their mission to provide expert, compassionate care could not be ignored, even in a pandemic.
In most circumstances, hospice is provided wherever patients call home, allowing them to be comfortable in their final days. Immediate changes to already tight safety protocols were combined with quick implementation of telehealth with physicians, nurses, chaplains, and social workers.
“The 2012 report on Crisis Standards of Care from the Institute of Medicine, declared that ‘provision of palliative care in the context of a disaster with scarce resources can be considered a moral imperative of a humane society. That call to action was largely ignored in the first wave of this pandemic, but it is more real now than ever during ongoing threats of overwhelming local and regional surges in demand for palliative and hospice care.”
~ JAMA, September 21, 2020
Kansas City Hospice’s two hospice houses, however, would face a different challenge entirely. A hospice house is designed to provide short-term acute care when symptoms are too complex to be handled at home. Plus, it offers respite care when home caregivers need a break. What would happen if the family member of a home hospice patient contracted the coronavirus or a hospice house patient tested positive?
Prior to March 2020 both Kansas City Hospice House™ and NorthCare Hospice House offered 24/7 unlimited visitation. Family meals were provided by volunteers, who also helped the families with immediate needs. Walking in the gardens and family gatherings were everyday occurrences.
Along with other inpatient facilities throughout the Metro, the two hospice houses took the heartbreaking step of limiting visitors to two people when hospitals and other facilities were allowing none or one visitor. All visitors and staff were provided with PPE and were screened at the door. Staff wore masks at all times. For those family members who could not safely visit, Zoom visits between patients and family members were offered. The three negative-pressure rooms were updated to ensure readiness for patients who might become COVID-positive.
 “We have done so much to ensure the safety of our patients and families while preserving the sanctity of being there at time of death with a loved one,” states Paul Weddle, COO of Kansas City Hospice.
“We have done so much to ensure the safety of our patients and families while preserving the sanctity of being there at time of death with a loved one,” states Paul Weddle, COO of Kansas City Hospice.
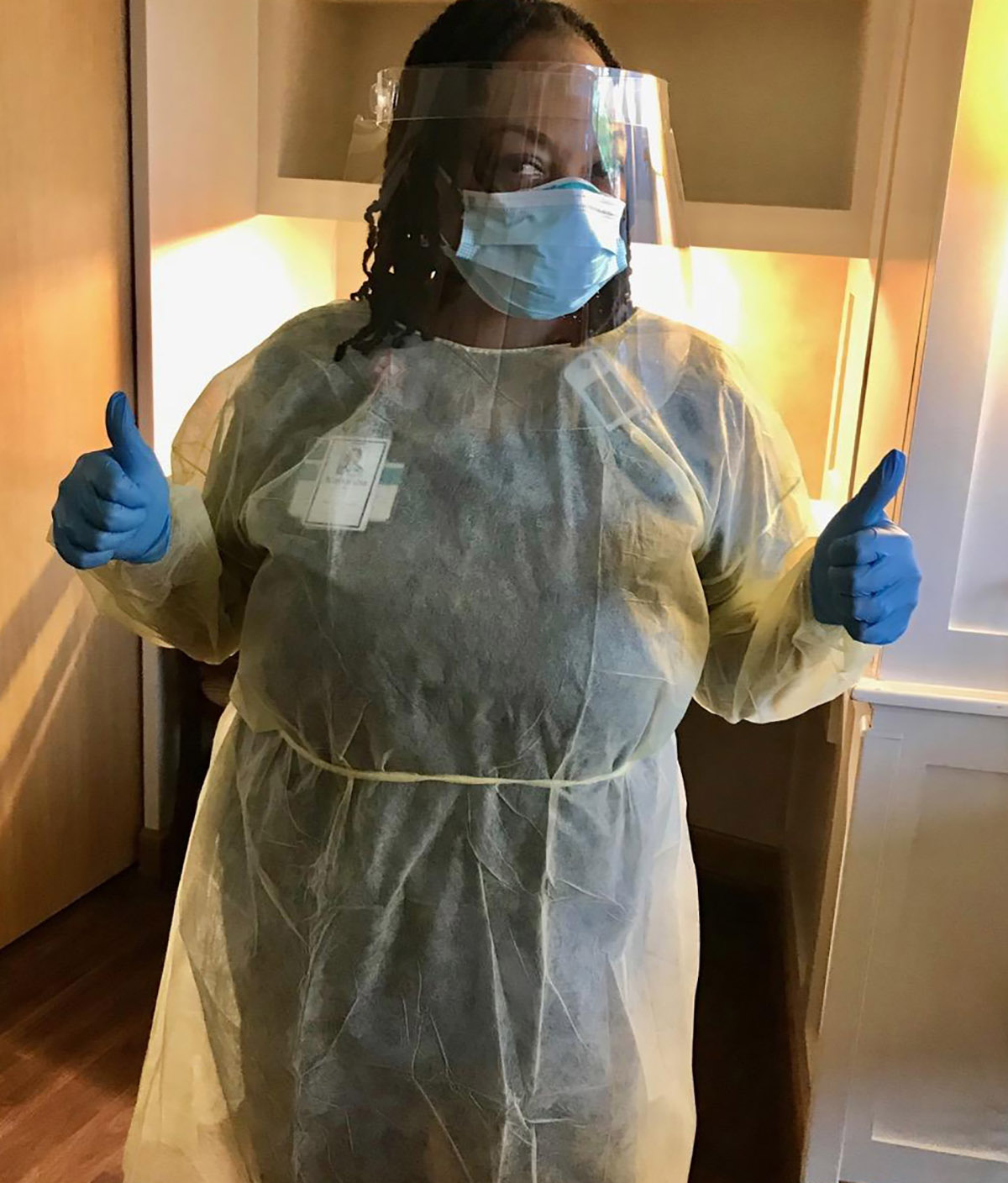
It was not going to be enough. Soon they began aerosolized precautions for patients on nebulizer treatments and high flow oxygen needs. The staff protocol changed from just mask to masks at all times plus full-face shields when within six feet of patients or visitors. All visitors were required to wear a mask upon arrival.
To offer more compassionate care, Kansas City Hospice House implemented patio visits for up to 10 visitors for 30 minutes. This allowed extended family a chance to be with their loved ones and allowed the opportunity to say their goodbyes if circumstances inferred it was time. NorthCare Hospice House is on the campus of North Kansas City Hospital and worked with hospital staff to provide visits within their guidelines. Some families had not seen their loved one for many months, coming out of a facility under lockdown protocols, and Kansas City Hospice House was grateful they could offer this opportunity to the families.
 “One patient was estranged from two sons,” notes Jeni Davenport, RN, KCHH Supervisor. “They were able to have a patio visit and make amends. It was so beautiful to see them all sitting out on the patio together laughing and talking. All of them were crying as they parted and the patient was very thankful for that special time.”
“One patient was estranged from two sons,” notes Jeni Davenport, RN, KCHH Supervisor. “They were able to have a patio visit and make amends. It was so beautiful to see them all sitting out on the patio together laughing and talking. All of them were crying as they parted and the patient was very thankful for that special time.”
Birthday celebrations on the patio included a patient who was turning 100. The staff hung a “happy birthday” banner between two IV poles. The families were especially thankful for those last precious moments they could spend together. Hospice house staff were honored to be able to make this a sacred moment. They strongly believe that the care they give is not just for patients, but for the entire family.
 “During a rainstorm one afternoon a family was considering rescheduling their visit,” recounts Denyse Hite, BSN, RN, Director of Inpatient Services. “Sensing that time was short, a nurse took off her shoes and rolled up her pant legs to run out in the rain with an umbrella. She brought the family up to the patio, where they were able to be with their loved one for the last moments.”
“During a rainstorm one afternoon a family was considering rescheduling their visit,” recounts Denyse Hite, BSN, RN, Director of Inpatient Services. “Sensing that time was short, a nurse took off her shoes and rolled up her pant legs to run out in the rain with an umbrella. She brought the family up to the patio, where they were able to be with their loved one for the last moments.”

Eventually they were able to adapt and expand to four designated visitors. Then, rising numbers of coronavirus cases made it necessary to decrease the number of patio visitors to four (not including those on the designated visitor list). Visits are made in an enclosed area separate from patients and staff members to allow those visits despite the cold weather.
The skilled and dedicated staff of both hospice houses are passionate about end-of-life care. The physicians, nurses, aides, social workers and chaplains continue to work to make the experience meaningful to the families in their care, despite the hazards of a pandemic.
 Pamela Harris, MD, FAAPMR, FAAHPM, is the Director of Medical Programs for Kansas City Hospice, who has worked as an integral part of the COVID Task Force to create the necessary changes. “One thing that has not changed is the exceptional, compassionate care that the people of Kansas City Hospice provide each patient and family,” relates Dr. Harris, “Our people have been brave, resourceful, and amazingly resilient through this challenge They have worked tirelessly to help families say their goodbyes. It’s what we do.”
Pamela Harris, MD, FAAPMR, FAAHPM, is the Director of Medical Programs for Kansas City Hospice, who has worked as an integral part of the COVID Task Force to create the necessary changes. “One thing that has not changed is the exceptional, compassionate care that the people of Kansas City Hospice provide each patient and family,” relates Dr. Harris, “Our people have been brave, resourceful, and amazingly resilient through this challenge They have worked tirelessly to help families say their goodbyes. It’s what we do.”






