GO PURPLE

For Lupus Awareness Month 2018!
Lupus is a rather complex disease that can initially present in any number of physical manifestations. As a result, without specific tests performed on the patient, it can be challenging to diagnose in its early stages. Still, this chronic condition is quite the heavy hitter when it comes to how it plagues the body. Thanks to Lupus Awareness Month in May, both patients and medical professionals alike are given a platform by and through which to learn so much more about this disease, how to diagnose it, treat it and ultimately live with it.
Clinically described, lupus is a chronic autoimmune disease that can damage any part of the body, including the skin, joints and/or organs. Chronic is a term typically described when any signs or symptoms extend beyond six weeks and often for many years. With the onset of lupus, the immune system, the part of the body responsible for fighting off viruses, bacteria and germs, goes haywire. A normal immune system will produce proteins, referred to as antibodies, to protect the body from such harsh invaders. An autoimmune disease like lupus essentially translates that system into a language the body cannot read, and as a result, the immune system cannot distinguish between the foreign invaders and the body’s own healthy tissues. In this process, it will create certain autoantibodies that attack and destroy the healthy tissue.

Dr. Magaden talking with patients
It is important to note, however, that lupus is not contagious. You cannot catch it from someone nor can you give it to someone. This disease is not like or even related to cancer, either. It is strictly an autoimmune disease that relies on treatment options such as therapies used to treat lupus, including NSAIDS, corticosteroids, antimalarials, immunosuppressives, anticoagulants and monoclonal antibodies/biologics. The symptoms of lupus can very, from mild in presentation to life-threatening. It is a condition that should always be treated by a doctor, and with solid medical care, most people with lupus can lead a full life.
It is estimated that at least 1.5 million Americans have lupus and that five million people throughout the world have a form of lupus. This disease typically strikes women of childbearing age. However, men, children and teenagers can also develop this disease. The average age for development of this disease is between 15-44. Women of color are up to three times more likely to develop lupus than Caucasians, but people of all races and ethnic groups can develop lupus.
Lupus can affect the patient in a myriad of ways, and the signs and symptoms are wide and varied. The symptoms may come and go, as well, and different symptoms may appear at different times during the course of the disease.
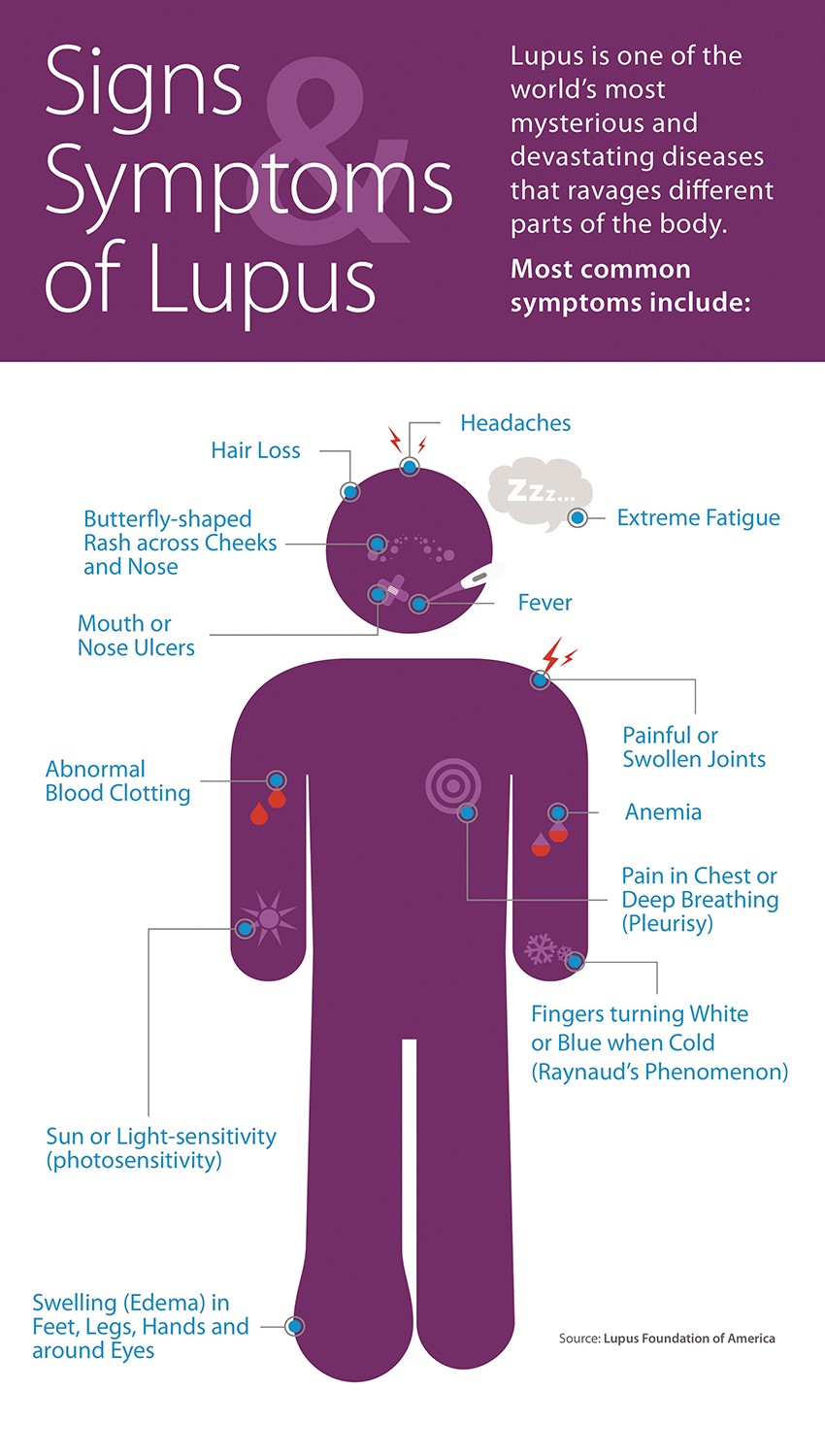
Among the common symptoms of lupus are extreme fatigue, painful or swollen joints, headaches, fever, anemia, edema, hair loss, sensitivity to the sun or to light, pleurisy, butterfly-shaped rash across the cheeks and nose, abnormal blood clotting, ulcers in the mouth or nose, and fingers that turn white and/or blue when cold (known as Raynaud’s phenomenon).
Risk factors for lupus include your sex, as women are more likely to develop lupus than men; your age, as symptoms of lupus typically occur between the ages of 15 and 44; your ethnicity, as in the United States, lupus is more common in people of color than in the Caucasian population; and your family history, as relatives of those with lupus have up to a 13% chance of developing lupus.
Additionally, there are four types of lupus: systemic lupus erythematosus; cutaneous lupus erythematosus, drug-induced lupus erythematosus; and neonatal lupus. Systemic lupus is the most common. Cutaneous lupus is limited to the skin. Drug-induced lupus is a lupus-like illness caused by certain prescription drugs; and neonatal lupus, not necessarily a true form of lupus, is a rare condition affecting infants of women who have lupus caused by antibodies that affect the infant while in the womb.
Thanks to the Lupus Foundation of America – Heartland Chapter, patients and caregivers alike can benefit from the programs and services this national organization provides to improve the quality of life for all of those affected by lupus. Through ongoing research, education, support and advocacy, the Lupus Foundation regularly brings together experts on this disease, implements strategies, provides resources and rallies support across the country to help solve the mystery of this illness.
One of the trusted and respected resources relied upon by The Lupus Foundation of America-Heartland Chapter is Julian Magadan, III, a rheumatologist at The Center for Rheumatic Disease. Dr. Magadan earned his medical degree from the University of Texas Southern Medical school and is one of seven doctors who specializes in Rheumatology. A strong believer in patients advocating for themselves, Dr. Magadan is passionate about educating others about this disease and encouraging them to do their own research and partnering with their primary care physician early on in the event they present with any symptoms that might be suspicious.
“Lupus is an autoimmune disease in which the immune system attacks healthy cells by mistake, which can then damage many other parts of the body,” noted Dr. Magadan. “Your immune system creates proteins that don’t protect you but, instead, target your organs. This, in turn, can manifest in various ways through problems with the skin, kidneys, heart, and lungs.”
Lupus affects people differently. Some patients may only present with a few mild symptoms while others may struggle with more several symptoms. The symptoms can begin in early adulthood, between the teen years and into the 30s. With lupus, patients typically experience flare ups followed by periods of remission. As such, the early symptoms are often missed. In fact, lupus has been referred to as the great imitator, as many of its symptoms often mimic other diseases.
“According to the College of Rheumatology, patients must meet a minimum of four out of 11 criteria to meet the diagnosis of lupus,” explained Dr. Magadan. Among the most prevalent symptoms are ulcers of the mouth and nose; a butterfly rash on the face; protein or blood in the urine; color changes in the hands; abnormal antibodies; recurrent miscarriages; blood clots; gastrointestinal issues, thyroid problems; fatigue; fever; and even hair loss. It is not uncommon for new symptoms to appear while others disappear. As such, it can be challenging to diagnose this disease early, as the symptoms can be mistaken for other issues. Further, these symptoms may occur for six months to a year before the disease is even diagnosed.
Dr. Magadan noted that lupus is not as common in men as it is in women, and that it tends to present differently depending on one’s ethnicity.
“The typical African American patient may have blood in the urine, heart issues, cough up blood, or problems with the kidneys or lungs,” he indicated. “On the other hand, a Hispanic patient’s initial symptom may be blood in the urine and a Caucasian may experience joint pain and fatigue.”

The Kansas City Walk to End Lupus Now is scheduled for September 15, 2018
Without a cure, how is lupus treated? According to Dr. Magadan, it depends primarily on the manifestations of the disease. Additionally, a patient may present with one or two symptoms initially but over time, symptoms are additive and there is the chance the disease can progress to affecting other parts of the body.
“With mild cases, a first line of therapy for lupus patients is the drug Plaquenil. For the moderate to severe cases, we use a more aggressive approach with agents such as Cellcept, Imuran in combination with Plaquenil,” said Dr. Magadan. “Lupus is a lifelong disease, but once a patient is on therapy, he or she begins to feel better and we expect to see a good response to the medications. However, some patients that have had kidney failure can end up on dialysis.”
Current medicinal therapies for lupus include Plaquenil, Methotrexate, Imuran, Cellcept, Arava. A future therapy currently under study includes Rituxan. Nevertheless, since lupus is a highly complex illness, Dr. Magadan suggested there is some hesitation with respect to more advanced therapies on the horizon.
“Lupus treatment is lacking in the area of new medications,” he commented. “The complexity of the disease makes limited movement with respect to more advanced therapies.”
With May as Lupus Awareness Month, this is a great time to cast a strong spotlight on this disease, the people it affects, and how to take positive action in terms of treatment, overall care, and living with this disease. Listen to your body. Ask questions. Stay involved with your care. It’s up to you to help your doctor help you manage this disease.
Join the Lupus Foundation of America – Heartland Chapter – as it promotes this awareness initiative through a variety of endeavors. On May 18th, everyone is encouraged to wear purple for Put on Purple Day. Snap a selfie and upload it to Facebook, Instagram and Twitter with #PutonPurple or #POP. The following day, the St. Louis Walk to End Lupus Now will be held to increase awareness of the disease and to raise funds for lupus research. Here in the metro area, the Kansas City Walk to End Lupus Now will occur on September 15, 2018.
The Heartland Chapter will participate in community events to bring further awareness to lupus by distributing educational materials and the Chapter will post a calendar of lupus awareness events taking place throughout the Chapter territory on its website.
Julian Magadan, III, M.D. of the Center of Rheumatic Diseases
4330 Wornall Rd., Suite 40, Kansas City, MO 64111 | (816) 531-0930







