Prostate Cancer

Early Detection is Essential
What is Prostate Cancer?
Cancer can start any place in the body. Prostate cancer is a cancer that occurs in the prostate — a small walnut-shaped gland in the male reproductive system. When a mutation in one of the glands of the prostate occurs, a cancer develops and grows, ultimately leading to symptoms. Usually prostate cancer grows slowly and is initially confined to the prostate gland, where it may not cause serious harm. However, some grow relatively quickly and may spread from the prostate to other areas of the body, such as the bones and lymph nodes. Prostate cancer that’s detected early — when it’s still confined to the prostate gland— has a better chance of successful treatment. Due to increasing life expectancy and the introduction of prostate-specific antigen (PSA) screening, a rising number of elderly men are diagnosed with prostate cancer.
 What are early warning signs of Prostate Cancer?
What are early warning signs of Prostate Cancer?
Dr. Peter J. Van Veldhuizen, MD, a board-certified, fellowship trained hematology/medical oncology physician serving patients in the Greater Kansas City region states that “The most common signs are; increasing difficulty in urination or going to the bathroom. The urine stream can slow and be difficult to get started; less commonly there can be pain and discomfort with urination or pain with urination or pain in the pelvic area.” Dr. Van Veldhuizen specializes in Genitourinary (GU) malignancies and sees patients at Sarah Cannon Cancer Institute at Menorah Medical Center. Other symptoms can range from blood in the urine (Hematuria), frequent urges to urinate at night and even loss of bladder control. Sometimes it is associated with difficulty getting an erection (erectile dysfunction), painful ejaculation and blood in the semen. If you have any of these symptoms you should have your doctor perform a couple of standard screening tests. The first is a digital rectal exam (DRE) test that allows a doctor to check the lower rectum, pelvis, and lower belly for the cancer. If your doctor finds any abnormalities in the texture, shape or size of the gland, you may need further tests. The second test is a Prostate-specific antigen (PSA) test where blood is drawn from a vein in your arm and analyzed for PSA. PSA is a substance that is naturally produced by your prostate gland which is found in your bloodstream even when you are healthy. However, if a higher than normal level is found, it may indicate prostate infection, inflammation enlargement or cancer. If a DRE or PSA test detects an abnormality, your doctor may recommend further tests. These tests help you and your doctor make informed decisions about your treatment.
Is Prostate Cancer fatal?
Approximately 90% of all prostate cancers are detected in the local and regional stages, so the cure rate is very high: Nearly 100% of men diagnosed and treated at this stage will be disease-free after five years. However, Dr. Van Veldhuizen says, “Many men do have slower growing prostate cancers which are frequently not fatal; prostate cancer is still the second most common cause of cancer deaths in many, with only lung cancer being a more common cause.”
What are the chances of surviving Prostate Cancer?
According to Dr. Van Veldhuizen, “The chance of surviving prostate cancer are dependent on the stage and how early the cancer is found. Patients with early stage (stage I or II) cancer have survival rates exceeding 80-90% depending on the specific circumstance. Patient with stage IV disease, or spread of the cancer to other areas, are not curable although with treatment patients can still live with the disease for many years.”
Viral etiology of prostate cancer. Conceptual illustration showing viruses infecting prostate gland and causing cancer development.
What are the signs that Prostate Cancer has spread?
Signs of spread vary from patient to patient but the most common early signs include fatigue or loss of energy, decrease in appetite, and pain in the bones.
What treatment options are available?
There is no “one size fits all” treatment for prostate cancer. Men diagnosed with localized prostate cancer may live for many years, it is important to discuss not only cure, but also quality of life.
A man diagnosed with localized or locally advanced prostate cancer has a variety of treatment options:
- Watchful & Active Surveillance – active surveillance is for patients who have a slow growing tumor where it is possible that even without treatment the cancer may not cause any issues for the lifetime of that patient. It is only for patients who on biopsy have evidence of a small amount of tumor or a less aggressive tumor on biopsy as measured by what is called the Gleason’s score. Gleason’s score is on a scale of 0-10 with 10 being the most aggressive. To be a candidate for active surveillance it should be 6 or less. Under this option, patients would be monitored every 3-6 months with a PSA and exam. A biopsy may be repeated after 1-2 years, only patients with a change in biopsy would then undergo treatment. If stable, then continue follow-ups. This approach allows a significant number of patients to avoid treatment and potential side effects without the risk of still undergoing curative treatment if the disease changes.
- Surgery – is the option of removing the prostate gland and the cancer. For early stage cancers, it has a high potential for cure. In some patients, side effects include incontinence or effect on sexual function. It is used only for early staged cancers.
- Radiation Therapy – is a treatment that uses high-energy rays to kill cancer cells or shrink tumors over 6-8 weeks.
- Proton Beam Radiation – is a treatment option that involves using a focused ray of proton particles to destroy cancerous tissues. The treatment can deliver precise, high doses of radiation to accurately target cancer cells without causing damage to healthy tissue surrounding the prostate.
- Hormone Therapy – is also called androgen deprivation therapy (ADT) or androgen suppression therapy. The goal is to reduce levels of male hormones, called androgens, in the body, or to stop them from affecting prostate cancer cells. Androgens stimulate prostate cancer cells to grow.
- Chemotherapy – is medication given by the vein which attacks the ability of the cancer to grow and divide. It is most commonly used when hormonal therapy stops working. Chemotherapy is given in cycles of treatment followed by a recovery period. The entire treatment generally lasts three to six months, depending on the type of chemotherapy medications given.
- Immunotherapy – is a broad category of cancer therapies that use the body’s immune system to fight cancer cells. These cells are different from normal cells, in that they do not die normally. Think of these rapidly-dividing cells like an out-of-control copy machine that won’t stop creating images. These abnormal cells frequently change, or “mutate,” to evade the immune system. Currently the only approved immunotherapy option is called Provenge which is a vaccine given every other week for three doses.
- Bisphosphonate Therapy – is the use of bisphosphonates to treat prostate cancer that has spread to the bone. Bisphosphonates can have side effects, including flu-like symptoms and bone or joint pain. They can also cause kidney problems, so patients with poor kidney function might not be able to be treated with these medicines.
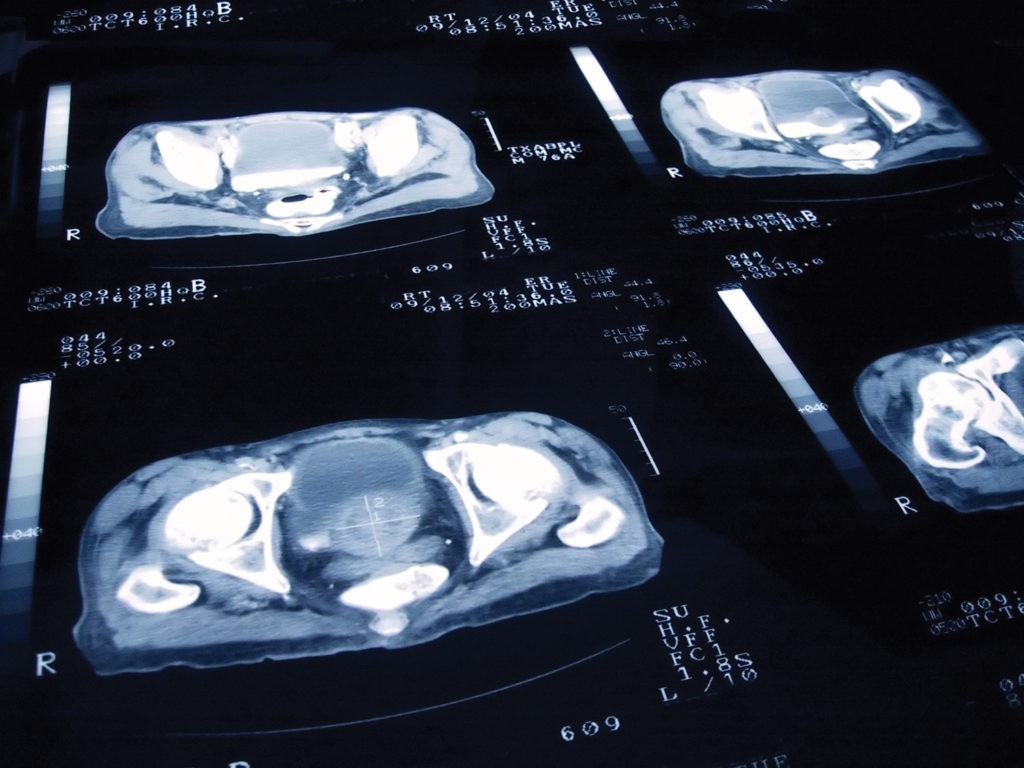
Prostate Ultrasound, this imaging test provides images of the prostate gland and surrounding tissue. The probe sends and receives sound waves through the wall of the rectum into the prostate gland which is located in front of the rectum.
Choosing the best treatment for localized or locally advanced prostate cancer is generally based on the man’s age, the stage and grade of the cancer, the man’s general health, and the man’s evaluation of the risks and benefits of each therapy option. Dr. Van Veldhuizen believes, “There is definitely hope, early stage disease is highly curable and patients with advanced disease can still live many years with treatment (and maintain a good quality of life). As we continue to research, there is still hope that this disease may be curable in all patients.”
The Sarah Cannon Cancer Institute at HCA Midwest Health is a network-accredited cancer program with seven area hospitals. Dr. Van Veldhuizen can be reached at Menorah Medical Center at (913) 489-7409. For more information on prostate and other genitourinary cancers visit hcamidwest.com/cancer.